Sam Van Alstyne, 3M Drug Delivery Systems 10.11.17
It is no secret that technology is transforming the landscape of drug delivery. In the last decade, we’ve seen a major shift in how we think about delivering drugs to patients, and we’re finding ways to solve problems that, until now, seemed unsolvable. While we’ve made great strides, the influence of digital technology on drug delivery is still in its infancy, and there are many hurdles to clear before we reach the finish line. Technology, by its very nature, is constantly evolving. Innovation never stops. While this is inherently a good thing, it can be a daunting task to try to keep up with it. What follows is a snapshot of where the world of drug delivery technology stands at this particular moment in time.
Patient empowerment
In attending several digital healthcare conferences each year, there is a real shift in how we think about using technology in the delivery of healthcare. Early on, the use of technology was focused on concepts like tele-medicine as a way to provide healthcare access to patients in underserved areas. Today, patient empowerment is at the center of the conversation surrounding healthcare and drug delivery technology. How can we use technology to augment existing care and provide the tools to allow patients to better manage their own condition?
Now, more than ever before, conference topics are focused on using consumer insights and user-centered design to create patient-centric products. It is encouraging that this mindset is becoming mainstream, because it will likely result in vastly improved patient care. Empowering patients to take back control of their own health, through the use of data and other insights, is a critical piece of the healthcare puzzle that has been missing for way too long. When we can help patients have the information they need, it may help them take action sooner rather than later, thus improving the situation overall.
As scientists and engineers begin drafting new designs for drug delivery methods, they are now starting with the patient at the ground level and working their way up. Historically, that has not been the case, and it has caused a disconnect that has inadvertently left patient circumstances out of the equation. The benefit of this new approach is the ability to first understand patient circumstances and the challenges they present. Technology makes it easier to address those issues on the front-end, with the goal to ensure better results on the back-end.
Patient adherence is one of those issues. You may think you have the best drug delivery system ever designed, but if the patient forgets to use it or uses it incorrectly, it isn’t going to do him/her any good. When it comes to inhalation therapy, for instance, patients often don’t use their inhalers correctly and may not even realize it. In fact, in a 2008 research report, up to 94% of patients make mistakes when using their inhalers—and these were dry powder inhalers, which were supposed to be easier to use.
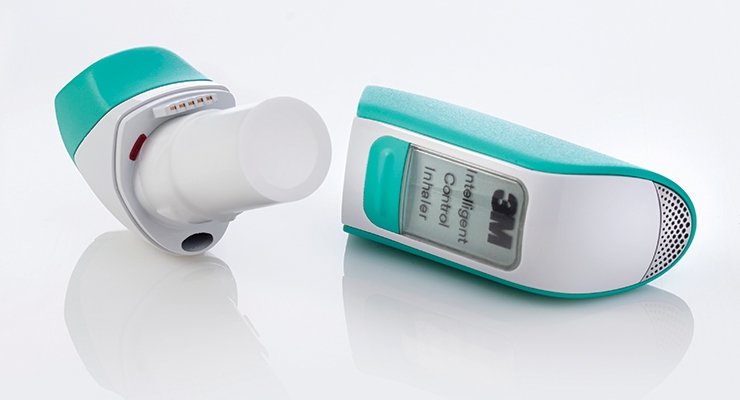
By building technology into drug delivery devices, we can help solve those problems. Sensing technology is built into the 3M Intelligent Control Inhaler that is currently in development. It is designed to detect whether a patient inhaled long enough to get the full dose of the drug. By connecting it to a smartphone or tablet, the device can also remind the patient to take the drug and instruct him/her on how to use it. Finally, it can record that data to help guide and improve future healthcare decisions.
The benefits of this technology may not only improve patient outcomes, it may also drive down healthcare costs, which is one of the major factors driving technological advancements in the healthcare industry. Currently, the cost of healthcare is unsustainable and only getting worse. We know preventive care saves money. By getting a drug more effectively and efficiently into a patient, we may prevent costly doctor visits, hospital stays, etc. I firmly believe that empowering patients in this way is key to reducing healthcare costs in the long-term.
Paying for It
Before we can get to that point, however, we’re faced with a major challenge: who’s going to foot the bill to get these new technologies into the hands of patients? That’s the billion dollar question right now.
On the front-end, the money is there to fund the development of new and innovative approaches to healthcare. According to Rock Health, for instance, in 2016, $4.2 billion was invested in digital health start-ups. At conferences, it is always amazing to see the incredibly creative solutions on display. The desire, drive and technology are there to do great things for patients.
However, beyond that point, the unfortunate reality is that most of these new discoveries and developments are struggling to survive in the marketplace. The question becomes, “How do we get these technologies from the development lab to the pharmacy counter?” We are missing the innovative business models that help turn these inventions into sustainable businesses.
Instinctively, we turn to the health insurance payers to pay to get these technologies into the hands of patients, because their traditional role has involved investing in ways to reduce the cost of care. However, ways to deliver care are evolving faster than the industry can adapt. Models based on share-of-savings are popular, but defining and proving what the savings are remains challenging. In order to move forward, we need to look beyond the payer and understand who benefits, how they benefit and find ways to partner.
When it comes to drug delivery in particular, we have an especially challenging situation since most, if not all, of the payer-quantified value comes from the molecule delivered, rather than the technology that delivers it. In other words, the full value of the solution is based on the drug itself with little to no “boost” for an innovative technology. Without innovation in the reimbursement model, there’s not a clear way to get that technology into the hands of the people that need it at scale.
Embracing It
Not only do we need to figure out how to get a high-tech drug delivery device into the hands of patients, we need to make sure patients and their healthcare providers are willing to embrace it. Whenever new technology is introduced, growing pains are inevitable. Learning how to use a new device takes time. It is a short-term investment for long-term gains of efficiencies and improved care, but, in their busy day-to-day lives, patients and providers may not always see it that way.
Among healthcare providers specifically, better ways of helping patients take the medication they need is often hailed as a great thing, but it presents yet another item on a growing to-do list. In most cases it is up to the healthcare provider to teach the patient how to use their drug delivery device properly. Of course, that first means the provider must be trained in how to use it. In respiratory alone there’s a complex mix of delivery technologies, so it can be a struggle for a healthcare provider to stay on top of it all. To be successful, a device must be easy to understand and simple to use. That benefits both the patient and the provider.
Due to these factors, when developing a new drug delivery technology, we must include input from patients and providers at all stages of development and make the process as easy for them as possible. When we talk to doctors, they tell us that sometimes technology is one more thing standing between them and their patients. Our challenge is to make sure digital drug delivery devices help the doctor-patient relationship, rather than hinder it.
Another challenge facing the digital drug delivery industry is high-profile hackers and security breaches. Currently, people are already cautious about sharing their personal information in the digital space. When it comes to sharing something as intimate and private as their health data, patients have reason to be reluctant. It is incumbent upon us to prove that they can trust us.
Approving it
Rapidly changing technology presents challenges at every stage of the drug delivery design process. The regulatory stage is no different. Currently, regulators are working to adapt their process to meet the challenges created by an ever-increasing pace of innovation and development while, at the same time, ensuring high standards for patient safety remain in place.
From a designer’s point of view, it can feel like you’re pushing water uphill. You wish it could all move faster. From a regulatory point of view, the top priority is being very, very careful to make sure the device enhancing the delivery of the medication will do no harm to patients. The process of approving drug delivery systems for patient use must be thorough. Currently, the two sides are working hard to find a balance, in order to achieve the common goal of getting new technology into the hands of patients as safely and as rapidly as possible.
What’s next?
There are many question marks in the digital drug delivery industry. The biggest one always has been and always will be: “What’s next?” In my opinion, one of the things we’re going to see in the not-too-distant future is targeted therapies for cancer patients.
For instance, technological advances in the area of inhalation drug delivery could bring drastic improvements to the fight against lung cancer. We know we have the ability to reach the lungs and put the treatment in the optimal place. As we see improved treatments, such as genetic matching of therapies to patients, the opportunities to help patients that once had little hope for survival will only continue to grow.
Conclusion
Over time, all drug delivery is going to be heavily influenced by technology. This is the future, plain and simple. At the end of the day, it is about getting the drug into the body in the most efficient and effective way possible. Technology will make that easier, more reliable, and ultimately provide better overall patient outcomes.
For me personally, it is fantastic to see technology and drug delivery come together. I started my career as a computer scientist at a time when healthcare innovation was centered on “big iron”—large, expensive systems focused on solving a narrow set of challenges. Now we’re using the phones in our pocket to bring that innovation to everyone.
Sam Van Alstyne is new products marketing manager at 3M Drug Delivery Systems.
Patient empowerment
In attending several digital healthcare conferences each year, there is a real shift in how we think about using technology in the delivery of healthcare. Early on, the use of technology was focused on concepts like tele-medicine as a way to provide healthcare access to patients in underserved areas. Today, patient empowerment is at the center of the conversation surrounding healthcare and drug delivery technology. How can we use technology to augment existing care and provide the tools to allow patients to better manage their own condition?
Now, more than ever before, conference topics are focused on using consumer insights and user-centered design to create patient-centric products. It is encouraging that this mindset is becoming mainstream, because it will likely result in vastly improved patient care. Empowering patients to take back control of their own health, through the use of data and other insights, is a critical piece of the healthcare puzzle that has been missing for way too long. When we can help patients have the information they need, it may help them take action sooner rather than later, thus improving the situation overall.
As scientists and engineers begin drafting new designs for drug delivery methods, they are now starting with the patient at the ground level and working their way up. Historically, that has not been the case, and it has caused a disconnect that has inadvertently left patient circumstances out of the equation. The benefit of this new approach is the ability to first understand patient circumstances and the challenges they present. Technology makes it easier to address those issues on the front-end, with the goal to ensure better results on the back-end.
Patient adherence is one of those issues. You may think you have the best drug delivery system ever designed, but if the patient forgets to use it or uses it incorrectly, it isn’t going to do him/her any good. When it comes to inhalation therapy, for instance, patients often don’t use their inhalers correctly and may not even realize it. In fact, in a 2008 research report, up to 94% of patients make mistakes when using their inhalers—and these were dry powder inhalers, which were supposed to be easier to use.
By building technology into drug delivery devices, we can help solve those problems. Sensing technology is built into the 3M Intelligent Control Inhaler that is currently in development. It is designed to detect whether a patient inhaled long enough to get the full dose of the drug. By connecting it to a smartphone or tablet, the device can also remind the patient to take the drug and instruct him/her on how to use it. Finally, it can record that data to help guide and improve future healthcare decisions.
The benefits of this technology may not only improve patient outcomes, it may also drive down healthcare costs, which is one of the major factors driving technological advancements in the healthcare industry. Currently, the cost of healthcare is unsustainable and only getting worse. We know preventive care saves money. By getting a drug more effectively and efficiently into a patient, we may prevent costly doctor visits, hospital stays, etc. I firmly believe that empowering patients in this way is key to reducing healthcare costs in the long-term.
Paying for It
Before we can get to that point, however, we’re faced with a major challenge: who’s going to foot the bill to get these new technologies into the hands of patients? That’s the billion dollar question right now.
On the front-end, the money is there to fund the development of new and innovative approaches to healthcare. According to Rock Health, for instance, in 2016, $4.2 billion was invested in digital health start-ups. At conferences, it is always amazing to see the incredibly creative solutions on display. The desire, drive and technology are there to do great things for patients.
However, beyond that point, the unfortunate reality is that most of these new discoveries and developments are struggling to survive in the marketplace. The question becomes, “How do we get these technologies from the development lab to the pharmacy counter?” We are missing the innovative business models that help turn these inventions into sustainable businesses.
Instinctively, we turn to the health insurance payers to pay to get these technologies into the hands of patients, because their traditional role has involved investing in ways to reduce the cost of care. However, ways to deliver care are evolving faster than the industry can adapt. Models based on share-of-savings are popular, but defining and proving what the savings are remains challenging. In order to move forward, we need to look beyond the payer and understand who benefits, how they benefit and find ways to partner.
When it comes to drug delivery in particular, we have an especially challenging situation since most, if not all, of the payer-quantified value comes from the molecule delivered, rather than the technology that delivers it. In other words, the full value of the solution is based on the drug itself with little to no “boost” for an innovative technology. Without innovation in the reimbursement model, there’s not a clear way to get that technology into the hands of the people that need it at scale.
Embracing It
Not only do we need to figure out how to get a high-tech drug delivery device into the hands of patients, we need to make sure patients and their healthcare providers are willing to embrace it. Whenever new technology is introduced, growing pains are inevitable. Learning how to use a new device takes time. It is a short-term investment for long-term gains of efficiencies and improved care, but, in their busy day-to-day lives, patients and providers may not always see it that way.
Among healthcare providers specifically, better ways of helping patients take the medication they need is often hailed as a great thing, but it presents yet another item on a growing to-do list. In most cases it is up to the healthcare provider to teach the patient how to use their drug delivery device properly. Of course, that first means the provider must be trained in how to use it. In respiratory alone there’s a complex mix of delivery technologies, so it can be a struggle for a healthcare provider to stay on top of it all. To be successful, a device must be easy to understand and simple to use. That benefits both the patient and the provider.
Due to these factors, when developing a new drug delivery technology, we must include input from patients and providers at all stages of development and make the process as easy for them as possible. When we talk to doctors, they tell us that sometimes technology is one more thing standing between them and their patients. Our challenge is to make sure digital drug delivery devices help the doctor-patient relationship, rather than hinder it.
Another challenge facing the digital drug delivery industry is high-profile hackers and security breaches. Currently, people are already cautious about sharing their personal information in the digital space. When it comes to sharing something as intimate and private as their health data, patients have reason to be reluctant. It is incumbent upon us to prove that they can trust us.
Approving it
Rapidly changing technology presents challenges at every stage of the drug delivery design process. The regulatory stage is no different. Currently, regulators are working to adapt their process to meet the challenges created by an ever-increasing pace of innovation and development while, at the same time, ensuring high standards for patient safety remain in place.
From a designer’s point of view, it can feel like you’re pushing water uphill. You wish it could all move faster. From a regulatory point of view, the top priority is being very, very careful to make sure the device enhancing the delivery of the medication will do no harm to patients. The process of approving drug delivery systems for patient use must be thorough. Currently, the two sides are working hard to find a balance, in order to achieve the common goal of getting new technology into the hands of patients as safely and as rapidly as possible.
What’s next?
There are many question marks in the digital drug delivery industry. The biggest one always has been and always will be: “What’s next?” In my opinion, one of the things we’re going to see in the not-too-distant future is targeted therapies for cancer patients.
For instance, technological advances in the area of inhalation drug delivery could bring drastic improvements to the fight against lung cancer. We know we have the ability to reach the lungs and put the treatment in the optimal place. As we see improved treatments, such as genetic matching of therapies to patients, the opportunities to help patients that once had little hope for survival will only continue to grow.
Conclusion
Over time, all drug delivery is going to be heavily influenced by technology. This is the future, plain and simple. At the end of the day, it is about getting the drug into the body in the most efficient and effective way possible. Technology will make that easier, more reliable, and ultimately provide better overall patient outcomes.
For me personally, it is fantastic to see technology and drug delivery come together. I started my career as a computer scientist at a time when healthcare innovation was centered on “big iron”—large, expensive systems focused on solving a narrow set of challenges. Now we’re using the phones in our pocket to bring that innovation to everyone.
Sam Van Alstyne is new products marketing manager at 3M Drug Delivery Systems.